We are a research clinic and have dealt and successfully treated thousands of cases of male infertility over the last 30 years.
Infertility is not that affects only women, men are also equally affected. Among infertile couples, 40 percent of the male partner is either the sole factor or a contributing factor to infertility.
Male infertility is caused by some problem in the male, due to which he is unable to deposit normal, healthy, sperms, in sufficient quantity in the female reproductive tract to fertilize the eggs.
What is andrology?
Andrology is the science of the male reproductive system associated with reproduction only.
In recent times Andrology has grown in response to the need to help infertile couples along with the development of laboratory technology and research facilities. The diagnostic tests available to the clinician are:
Semen Analysis
A semen analysis is a set of tests which tells is about the sperms and the functioning of accessory glands. It is routinely done to help evaluate male fertility. Some of the parameters routinely looked for male fertility are:
Sperm Count
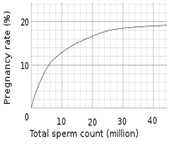
Sperm count= Sperm concentration x semen volume
Sperm count in million is directly related to pregnancy rate, and hence an important indicator of male fertility. With the advent of ICSI, this parameter has lost some of the significance in IVF procedures. WHO has lower limit of 20 million sperms for normal fertility.
A lower sperm count is termed oligozoospermia Near complete absence of sperm is termed azoospermia.
Motility
The WHO has a value of 50% and this must be measured within 60 minutes of collection. But if the total count is less than twenty million but high motility the fertility is considered good.
A more specified measure is motility grade, where the motility of sperm are divided into four different grades:
- Grade A or Motility IV: These sperms exhibit rapid straight line moment and are very strong and good for fertilization. These sperms are quite strong.
- Grade B or Motility III: These sperms also move forward but move in a circular fashion. These sperms also can fertilize the eggs.
- Grade C or Motility II: These sperms also move but do not show progressive movement. These sperms are not good for fertilization.
- Grade D or Motility I: These sperms, do not move at all, and are not good for fertilization.
Sperm Morphology
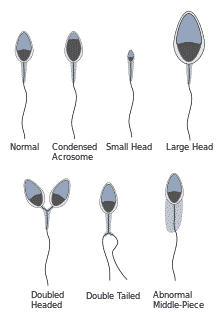
Morphology is a good predictor of success in fertilizing ability of oocytes during in vitro fertilization. Up to 10% of all spermatozoa have observable defects and as such are disadvantaged in terms of fertilizing an oocyte. Some of the sperm abnormalities are shown below.
Also, sperm cells with tail-tip swelling generally have lower frequency of aneuploidy.
A motile sperm organelle morphology examination (MSOME) is a particular morphologic investigation where a special microscope is used to magnify the sperm to X6000 to look for sperm large vacuoles, which indicate sperm chromatin immaturity.
Volume
According to WHO guidelines on semen analysis the semen volume varies from 1.5 ml to 4.0 ml. Semen volume less than 1.5 ml may indicate partial or complete blockage or absence of seminal vesicles.
Semen Color
Semen normally has a whitish-gray color. It tends to get a yellowish tint as a man ages. Presence of blood in semen (hematospermia) leads to a brownish or red colored ejaculate but it is a rare condition.
Some other causes of different color may indicate sexually transmitted diseases.
Fructose level
Fructose level in the semen may be analyzed to determine the amount of energy available to the sperm for moving. Fructose level of 13 u mol is considered normal. Absence or very low levels may indicate some problem with seminal vesicles.
pH
WHO specify normal pH as 7.2-7.8 a neutral acidity . An acidic or low pH semen may indicate one or both seminal vesicles are blocked. A basic semen (high pH) may indicate some infection. Any difference in pH from normal range affects the egg penetration ability of the sperm.
Liquefaction
The liquefaction is the process when the gel-like semen, is liquefied by enzymes in the semen. It normally takes nearly 20 minutes for a semen sample to liquefy. A liquefaction time within 60 minutes is regarded as within normal ranges.
MOT
MOT is a measure of how many million sperm cells per ml are highly motile at room temperature. This is a combination of both sperm count and motility. So for Intra-cervical insemination 0.5 ml volume should have 20 million motile sperms.
In WHO terms, it is thus recommended to use approximately 20 million sperms for IUI.
DNA Fragmentation
DNA damage in sperm cells is related to infertility and can be probed by analysis of DNA susceptibility to de-naturation in response to heat or acid treatment and/or by detection of DNA fragmentation revealed by the presence of double-strand breaks detected by the TUNEL assay.
Total motile spermatozoa Or total motile sperm count
Total motile sperms can be calculated by multiplying sperm count, motility and volume. It tells us how many motile sperms are present in a ejaculate.
Use of approximately 20 million sperm of motility grade C or D in ICI, and 5 million in IUI is an approximate recommendation.
Here are some common abnormalities of the semen /sperms
Abnormalities:
- Aspermia: absence of semen
- Azoospermia: absence of sperm
- Hypospermia: low semen volume
- Hyperspermia: high semen volume
- Oligozoospermia: Very low sperm count
- Asthenozoospermia: poor sperm motility
- Teratozoospermia: sperm carry more morphological defects than usual
- Necrozoospermia: all sperm in the semen are dead
- Leucospermia: a high level of white blood cells in semen.
New Technology that guides an andrologist:
Antisperm antibody assay
An antisperm antibody test which looks for special antibodies that fight against a man’s sperm in blood, vaginal fluids, or in the semen. The test is based on sperm agglutination when blood or vaginal fluid or semen is added to diluted sperms. Semen can cause antigen antibody response either in man’s or women’s body.
Sperm penetration assay
The sperm penetration assay (SPA), “hamster egg penetration test” (HEPT), is a in vitro test to
find the functional ability of the sperm to penetrate the human egg. This test is based on the ability of capacitated human sperm to penetrate zona free hamster eggs in vitro.
This test is superior to seminal fluid analysis in predicting both fertility and infertility. This test has application both clinically and experimentally.
Hemizona assay
This test is a diagnostic test to find the tight binding of sperm and zona pellucida of the egg to find fertilization ability of the sperm. This test is an excellent test to predict the outcome of IUI and IVF. So this test is very relevant as a diagnostic test for infertility.
Other Laboratory Techniques
There are a few more techniques which are used for improvement in semen storage and fertility treatments.
Sperm washing
Sperm washing is a procedure for separation of sperms from the semen. These washed sperms are used in IUI, IVF and ICSI.
Sperm “rise”
It is another procedure which involves the separation of healthy motile sperms for IVF-ICSI.
Cryopreservation
A frequently employed procedure is cryopreservation of sperms where the sperms are washed and stored in straws or vials for subsequent use in IUI, IVF or IVF-ICSI.
The andrology laboratory is a support service to a practitioner, a urologist and a reproduction specialist. With state-of-the-art technology, physicians are better able to address infertility, minimize patient distress and provide patients with reasonable options.
We performed our first sperm retrieval procedure in 1994. Since then we have been performing these procedures over the last 26 years and have more than 11000 babies in 55 countries.
Sperm retrieval/ Sperm extraction procedures
Sperm harvesting is different from a diagnostic testicular biopsy because, in this case, the aim is to find sperms in a patient who has no sperms in the ejaculate (azoospermia). In such patients the sperms have to be harvested directly from epididymis or testis.
Sperm retrieval procedure
There are several different procedures to retrieve sperms, depending on sperm production and blockage.
Summary of the procedures for sperm harvesting
Testicular sperm aspiration (TESA)
The simplest and most cost-effective procedure is sperm aspiration. This is performed under local anesthesia and takes approximately 10 minutes
The procedure is performed by inserting a needle with a syringe in the testis and aspirating fluid and tissue with negative pressure. The procedure, can be performed under local anesthesia, by any Obstetrician-Gynecologist in a operating theater or office setting. The procedure is generally coordinated with the female egg retrieval. TESA is performed for men with obstructive azoospermia (s/p vasectomy).
Some times TESA doesn’t provide enough tissue/sperm then an open testis biopsy is needed for sperm retrieval.
Testicular sperm extraction (TESE)
TESE is a little more complicated than TESA. It is a surgical procedure similar to testicular biopsy. It has to be performed by trained surgeon. There has always been debate, as to which procedure is “better” for obtaining sperm for successful intracytoplasmic sperm injection (ICSI). MicroTESE has replaced this procedure as the optimal form of sperm retrieval for men with no sperm in their ejaculate from a problem with production.
Precutaneous epididymal sperm aspiration (PESA)
PESA is a procedure for men with obstructive azoospermia, due to vasectomy or infection. This procedure is done under local anesthesia in operation theater or in the office setting coordinated with egg retrieval of the female.
Microdissection TESE (microTESE)
Micro TESE is a procedure performed on men who have problem with sperm production and are azoospermic. Micro TESE is performed in the operating room under general anesthesia with the help of operating microscope. Micro TESE is coordinated with the female partner’s egg retrieval. Micro TESE has significantly improved sperm retrieval rates in azoospermic men, and is also a safer procedure since less testicular tissue is removed. Patients can also opt for cryopreservation of sperm during this procedure for future IVF/ICSI.
Microepididymal Sperm Aspiration (MESA)
It is a procedure performed for men who have vasal or epididymal obstruction including vasectomy, congenital bilateral absence of the vas deferens. It can be done as a scheduled procedure or is coordinated with their female egg retrieval. MESA is performed in the operating room under general anesthesia utilizing the operating microscope. Patients can cryopreserve sperm during this procedure for future IVF/ICSI. it is a preferred method of retrieval of sperms for with congenital bilateral absence of the vas deferens.

 Your Journey to Parenthood Begins with us!
Your Journey to Parenthood Begins with us!